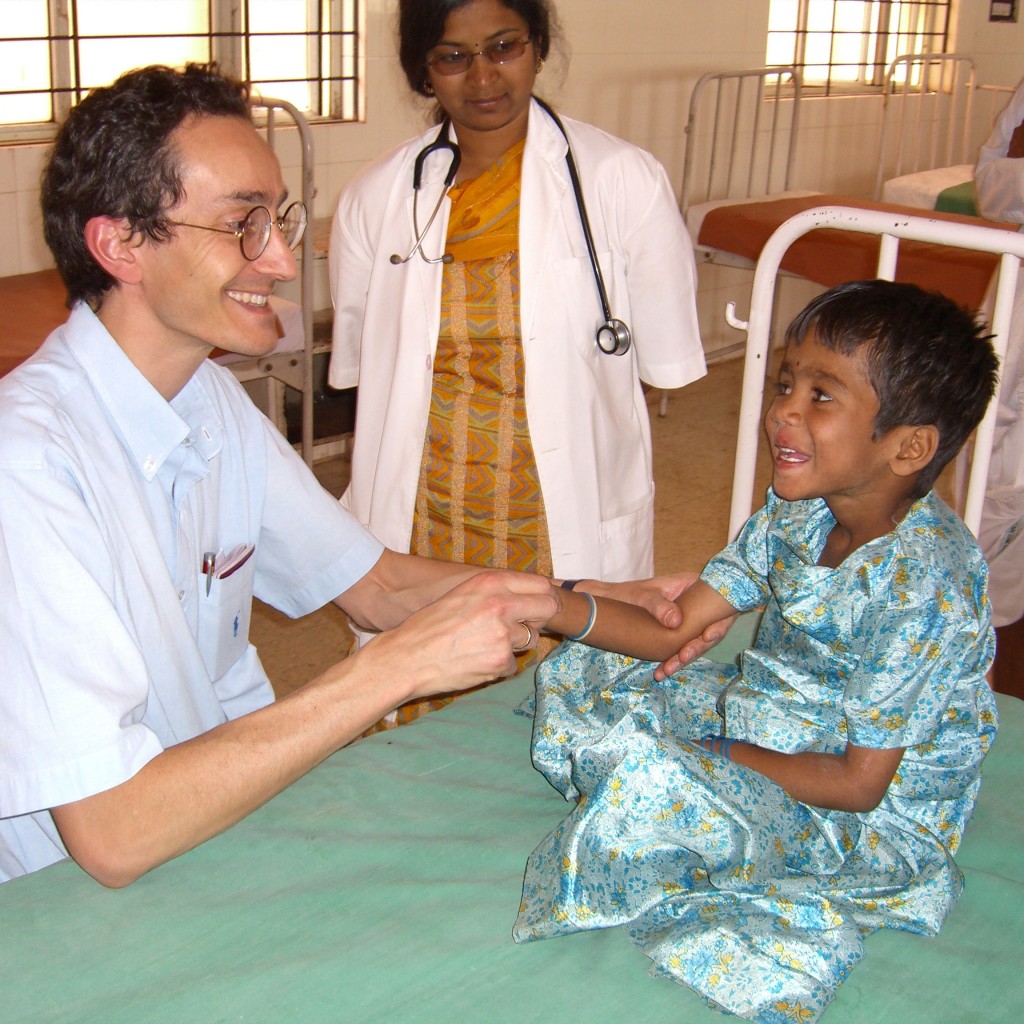
The Indian government has successfully immunised more than 100 million children against Japanese encephalitis
The World Health Organisation (WHO) will mark Immunisation Week this month to raise public awareness of how immunising against diseases such as measles, TB, and rotavirus, can save lives. Immunisation is one of the most successful health interventions in the world and prevents more than two million deaths every year.
Raising awareness of brain infections in India
More than 1,500 people, mostly children, died from an outbreak of ‘brain fever’ in India in 2005.
The disease, called Japanese encephalitis, is found in pigs and wading birds and is transmitted to humans by mosquitoes. It attacks the brain causing inflammation and swelling, resulting in seizures, brain damage, and in severe cases, death.
More than five years after the outbreak, India’s government, has successfully immunised more than 100 million children against the disease, with the support of researchers, charitable trusts and funding agencies from around the world.
Professor Tom Solomon (pictured) and Dr Lance Turtle have played a significant role in the vaccination of more than 50 million people against Japanese encephalitis
Researchers at the University of Liverpool have supported vaccine programmes across India for more than a decade and work closely with the Indian Institute of Science and the National Institute of Mental Health and Neurosciences (NIMHANS) in Bangalore on vaccine programmes and diagnosis tools.
Professor Tom Solomon and Dr Lance Turtle from the University’s Institute of Infection and Global Health, have played a significant role in the vaccination of more than 50 million people against the zoonotic disease and are currently working to develop blood tests to improve diagnosis of the disease.
Dr Turtle, who is based in Bangalore, is working to assess the health impacts of this serious illness on communities across Asia. The team is also investigating other causes of encephalitis and how the body responds to the disease.
Vaccinating children against malaria and rotavirus in Africa
The Institute is also part of an international consortium investigating the body’s immune response to a candidate malaria vaccine in newborn babies in Africa.
Malaria is a life-threatening parasitic infection, resulting in more than 200 million reported cases each year and approximately 800,000 deaths. In Africa a child dies of malaria every 45 seconds and the disease accounts for 20% of all childhood deaths.
The vaccine, RTS,S, developed by GlaxoSmithKline (GSK) Biologicals and PATH Malaria Vaccine Initiative (MVI), is currently in phase III clinical trials and has previously reduced episodes of malaria in infants and young children by more than 50%.
The Liverpool team, in collaboration with the University College of Medicine, Malawi, is working in Blantyre investigating how to maximise its effectiveness when delivered through the childhood immunisation programme.
Professor Nigel Cunliffe and the team are examining the performance of the vaccine as it is administered to infants at different stages between birth and nine months of age, alongside the standard set of immunisations used in national programmes for young children.
Professor Tom Solomon, head of the Institute of Infection and Global Health, said: “The work that we do is as much about scientific discovery in the lab as it is working with communities and learning about their experiences. These diseases are complex and can change in relation to a number of factors, such as climate, so working, living, and knowing the local community are key to the success of immunisation programmes.”
Other vaccine programmes include rotavirus infection in Malawi, where researchers have found that vaccination can significantly reduce the number of deaths from diarrhoea in infants, and testing new vaccine candidates for Streptococcus pneumonia.
The WHO Immunisation Week begins on the 22 April. For more information please visit: http://www.who.int/campaigns/immunization-week/2013/en/index.html